What it is:
Melanoma is the most serious type of skin cancer. It develops in the pigment producing cells in the skin known as melanocytes. Most melanoma begins on the surface of the skin where it is usually easy to see and treat. Sometimes, melanoma forms in areas that are hard to see, such as under hair, on soles of feet, or in the groin. Though rare, melanoma can also form in your eyes or internal organs. If given time, melanoma can grow deep into the skin, get into the bloodstream and travel to other parts of the body. This spreading (metastasis) can cause life-threatening illness. Melanoma is usually curable when detected early, but can be fatal if allowed to grow and spread.
What it looks like:
Melanoma is usually brown or black in color, but sometimes may be red, flesh-colored, or white. It can arise from a pre-existing mole, or appear as a new spot on the skin. When looking at your skin, it is helpful to apply the ABCDE rules:
(Source from: American Academy of Dermatology)
 |
Asymmetry: One half of the mole does not match the other half. |
 |
Border irregularity: The edges are ragged, notched, irregular, or blurred. |
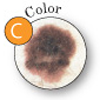 |
Color: The color is not the same throughout or it has shades of tan, brown, black, red, white, or blue. |
 |
Diameter: The mole is greater than 6 millimeters (¼”) in size, about the size of a pencil eraser. |
 |
Evolving: Spots that show any of these changes over time: Size, shape, shades of color; sensation (itching or tenderness); surface bleeding. |
How we find it:
If the doctor suspects that a spot on the skin is melanoma, the patient will need to have a biopsy. A biopsy is the only way to make a definite diagnosis. In this procedure, the doctor tries to remove all of the suspicious-looking growth. This is an excisional biopsy. If the growth is too large to be removed entirely, the doctor removes a sample of the tissue. The doctor will never "shave off" or cauterize a growth that might be melanoma.
A biopsy can usually be done in the doctor’s office using local anesthesia. A pathologist then examines the tissue under a microscope to check for cancer cells. Sometimes it is helpful for more than one pathologist to check the tissue for cancer cells.
When caught early, most skin cancer is very treatable. To maintain good skin health, most people should have their skin examined by a professional every year. In the meantime, you can do a skin self-exam every month. LEARN HOW HERE.
How we treat it:
Treatment for melanoma begins with the surgical removal of the melanoma and some normal-looking skin around the growth. Early melanoma limited to the outermost layer of the skin is known as melanoma in situ (in place), and simple surgical removal produces almost a 100 percent cure rate. If left untreated, the melanoma grows deeper in the skin and is more likely to become life-threatening.
Deeper melanomas can reach a blood vessel or lymphatic channel and spread. When a melanoma spreads, it goes to the lymph nodes first. The lymph nodes are part of the lymphatic system, a series of vessels throughout the body that are responsible for cleaning the body's tissue. It may be possible to find the melanoma in the lymph node before it goes any farther. A procedure called a sentinel lymph node biopsy is a way of identifying and testing the first lymph node into which the melanoma drains. The decision to perform a sentinel lymph node biopsy is based on how deep the melanoma is in the skin, and how likely it is to have spread. If the melanoma has spread to the lymph nodes, a complete lymph node dissection involving removal of all the lymph nodes in the area where the melanoma drains will be performed.
After the lymph node biopsy or dissection, treatment with radiation, chemotherapy or immunotherapy should be considered. Coordination of care with an oncologist and a dermatologist for frequent skin checks, chest x-rays and a LDH blood test should be done. Diagnostic imaging techniques such as x-ray, computed tomography (CAT scan), magnetic resonance imaging (MRI), positron emission tomography (PET scan) and radio-isotopic bone or organ scan may be included.
Call (520) 694-2873 for an appointment
Source: National Cancer Institute (http://www.cancer.gov)


